Table of contents
The process of diagnosing Polycystic Ovary Syndrome (PCOS) can be quite obscure, not only for patients but also for healthcare professionals. However, putting a name to your symptoms allows for a more effective approach to managing them as quickly as possible.
What is polycystic ovary syndrome (PCOS)?
PCOS, also known as Stein-Leventhal syndrome or ovarian dystrophy, is a hormonal disorder that affects between 10% and 13% of women. The root cause is a hormonal imbalance, which can stem from both ovarian and/or pituitary origins. This imbalance often disrupts the development of ovarian follicles, leading to an excess of immature follicles that accumulate in the ovaries. This buildup gives the ovaries a so-called “polycystic” appearance, though in reality, the term “multifollicular” would be more accurate, as these are follicles, not cysts.
PCOS is the leading cause of infertility in women and is commonly associated with hyperandrogenism. It is often linked with insulin resistance, which increases the risk of developing diabetes threefold.
PCOS is a complex syndrome that presents differently in every woman, but there are typically shared characteristics.
👉 Want to learn more about this condition? Read our full guide to PCOS here.
Common symptoms of PCOS
It’s important to remember that every woman is unique. Not all cases of PCOS are the same, but some or all of the following symptoms are frequently observed:
- Acne
- Excessive hair growth
- Hair loss
- Irregular or absent menstrual cycles
- Infertility (How to get pregnant with PCOS)
- Unexplained weight gain (How to lose weight with PCOS)
- Cravings for sugary foods
- Chronic fatigue (Managing PCOS stress)
- Headaches
If you find yourself identifying with several of these symptoms, it might be time to have a conversation with your gynaecologist, midwife, or general practitioner. In some cases, your gynaecologist may refer you to an endocrinologist, a specialist in hormonal health, for a thorough diagnosis.
The Diagnostic Process for PCOS
When you visit a healthcare professional, they will conduct a comprehensive assessment, which typically includes:
- Reviewing the diagnostic criteria for PCOS, known as the Rotterdam criteria.
- Assessing any potential metabolic issues, such as insulin resistance. While this step is not essential for diagnosis, it can provide valuable insight into your condition.
- Ruling out other conditions that present symptoms similar to those of PCOS.
The Rotterdam criteria
The International PCOS Network has updated the diagnostic recommendations for 2024.
After ruling out other conditions, the presence of two out of the three Rotterdam criteria is sufficient to confirm a diagnosis of PCOS:
- Irregular menstrual cycles and/or absence of ovulation
- Multifollicular ovaries observed via ultrasound or elevated Anti-Müllerian Hormone (AMH) levels in adults. This criterion is optional if there are menstrual irregularities along with hyperandrogenism.
- Clinical hyperandrogenism (such as hirsutism, acne, or androgenic alopecia) and/or biological hyperandrogenism (elevated androgen levels in blood tests).

What blood tests are necessary for a PCOS diagnosis?
This blood test, prescribed by your healthcare professional, is crucial. It allows for a complete diagnosis and rules out other hormonal disorders with symptoms similar to PCOS.
A blood test, ordered by your healthcare provider, is a crucial part of the diagnostic process. It helps confirm the diagnosis and rule out other hormonal disorders that may mimic PCOS:
- Androgen levels - including Testosterone, DHEA, and Delta 4: Elevated levels can cause acne, excessive hair growth, and hair loss.
- Anti-Müllerian Hormone (AMH): typically elevated in PCOS cases. However, it is not always tested, as there is no consensus on the minimum concentration threshold.
- LH, FSH, and estradiol levels: High levels of LH are often indicative of PCOS.
- Prolactin levels: for differential diagnosis purposes. This helps in excluding other conditions. Elevated prolactin levels may explain the absence of ovulation.
- Free cortisol levels: To rule out Cushing's syndrome.
- 17-hydroxyprogesterone levels: to rule out congenital adrenal hyperplasia (elevated 17 OH levels may require further testing to confirm or rule out this condition).
Once the hormonal tests are completed and the results are in, your endocrinologist or gynaecologist will explain the findings and confirm the diagnosis.
Ultrasound for PCOS diagnosis
An ultrasound is not required if a woman presents with irregular cycles and clinical or biological signs of hyperandrogenism.
When an ultrasound is necessary, it is usually performed transvaginally.
It is important to note that ultrasound is not recommended for adolescents, as multifollicular ovaries are common for up to eight years after the first menstrual period.
Ultrasound adds up to the diagnosis if one ovary contains at least 20 follicles measuring between 2 and 9 mm, or if the volume of one ovary is at least 10 mL.
Why is it important to pursue a full diagnosis?
While symptoms such as acne, excessive hair growth, weight gain, and irregular cycles may suggest PCOS, other conditions must be ruled out. Here are some of the conditions that need to be excluded when diagnosing PCOS:
- Hypothalamic Amenorrhea: This condition involves the cessation of menstrual periods due to a disruption in communication between the hypothalamus (a small region of the brain) and the ovaries. In summary, the hypothalamus stops producing GnRH hormones. This hormone acts as a messenger to stimulate the production of ovarian hormones LH and FSH. No communication means no ovarian hormones and therefore no cycle.
- Cushing's Syndrome: This condition causes significant hyperandrogenism and menstrual disturbances.
- Hyperprolactinaemia: elevated levels of the prolactin hormone are normal during pregnancy and breastfeeding but may cause irregular cycles, infertility, or reduced libido outside of these periods, making it easy to confuse with PCOS.
- Prolactinoma: A pathological form of hyperprolactinaemia may develop into a prolactinoma over time, a type of tumour representing 40% of all pituitary adenomas. This condition can cause visual disturbances, headaches, fatigue, menstrual irregularities, abnormal milk production outside of pregnancy/breastfeeding, infertility, and more.
- Congenital Adrenal Hyperplasia: This congenital condition can be mistaken for PCOS as it often causes hirsutism. It is associated with a deficiency in the enzymes responsible for steroid hormone synthesis, such as cortisol. Although typically diagnosed at birth, it may be detected later through the measurement of 17-hydroxyprogesterone, another hormone.
- Hypothyroidism: The thyroid gland is the conductor of your hormonal orchestra. When it is dysfunctional, symptoms such as a goitre (enlarged thyroid), fatigue, irregular periods, difficulty concentrating, weight gain, and loss of appetite may occur. Women with PCOS are often also affected by this condition, making it essential to have your thyroid hormones checked if there is any doubt.!
I’ve been diagnosed with PCOS, what next?
First, take a deep breath! Receiving a diagnosis can be overwhelming, so it’s important to surround yourself with supportive, caring people and to allow yourself to be pampered. Then, step by step, educate yourself about PCOS, because contrary to what you may hear, there are many, many ways to improve your quality of life with this syndrome. You might encounter discouraging perspectives, but rest assured, knowledge about PCOS is constantly evolving!
You might find our free e-book, which outlines the 10 commandments to manage your PCOS particularly helpful.
Here’s what you should know right away:
- PCOS does not make you sterile — natural fertility can return!
- A healthy lifestyle and appropriate supplements (like Ovastart and Sugar Balance) can help you manage your PCOS symptoms on a daily basis.
- If you're being asked to lose weight, consider checking for insulin resistance.
- The contraceptive pill is not the only solution.
- You don’t have to focus on your PCOS only when you want to have children.
- You have the right to seek a different healthcare professional if you feel you aren’t being heard.
- There are many highly knowledgeable doctors, gynaecologists, and midwives who specialise in PCOS!
- You are not alone. ❤️
✨ Feeling unsure where to start? Take the SOVA Product Quiz — it only takes 2 minutes and helps you find supplements tailored to your symptoms.
Educate yourself to better live with PCOS
Information is key! The more you know about your PCOS, the more empowered you will feel to take control of your health and the various ways you can address the condition.
Don’t give up—the journey is long, but it’s worth it. Congratulations for getting this far; you’ve already come a long way!
You’ll find plenty of support on our Instagram account, where you can connect with others who have been through the same experience, as well as access a wealth of information to keep learning.
At SOVA, we’re here for you too: to answer your questions, guide you, and support you—so don’t hesitate to reach out. 💜
- Polycystic Ovary Syndrome (PCOS) : A common hormonal condition affecting around 10–13% of women of reproductive age. It impacts ovulation, hormone balance, metabolism and, in some cases, fertility.
- Rotterdam criteria : The internationally recognised diagnostic criteria for PCOS. A diagnosis is made when at least 2 of the following 3 criteria are present: irregular or absent ovulation, signs of excess androgens, or polycystic ovaries on ultrasound.
- Hyperandrogenism : A state of excess “male” hormones (androgens) such as testosterone. It can cause symptoms like acne, excessive hair growth (hirsutism) or hair loss.
- Ovulatory dysfunction : Irregular or absent ovulation, often reflected by irregular menstrual cycles or missed periods.
- Polycystic ovaries / polycystic ovarian morphology : An ultrasound finding where the ovaries contain many small immature follicles. These are not cysts, despite the name.
- Insulin resistance : A metabolic condition in which the body does not respond properly to insulin, leading to higher insulin levels. It is commonly associated with PCOS and can increase the risk of type 2 diabetes.
- Hormonal blood tests : Blood tests used to assess levels of hormones such as testosterone, LH, FSH, prolactin or thyroid hormones, helping to rule out other conditions and support diagnosis.
- Endocrinologist : A medical specialist focusing on hormones and metabolic health, sometimes involved in PCOS diagnosis and management.
SOVA was created by two sisters with PCOS who wanted products that truly worked. Our formulas are developed in-house with women’s health and micronutrition experts, using ingredients backed by clinical studies and compliant with European regulations.
- Built by women with PCOS, we know the reality of the symptoms.
- Clinically studied, high-quality ingredients, including patented forms like Quatrefolic® and an optimal Myo-/D-Chiro Inositol ratio.
- Holistic support for hormonal balance, metabolic health, inflammation, mood and cycle regulation.
- Transparent, science-led formulas with no unnecessary additives.


Inositol Powder Supplement for PCOS


Berberine Supplement UK - Blood Sugar, Insulin & Metabolic Support for Women with PCOS

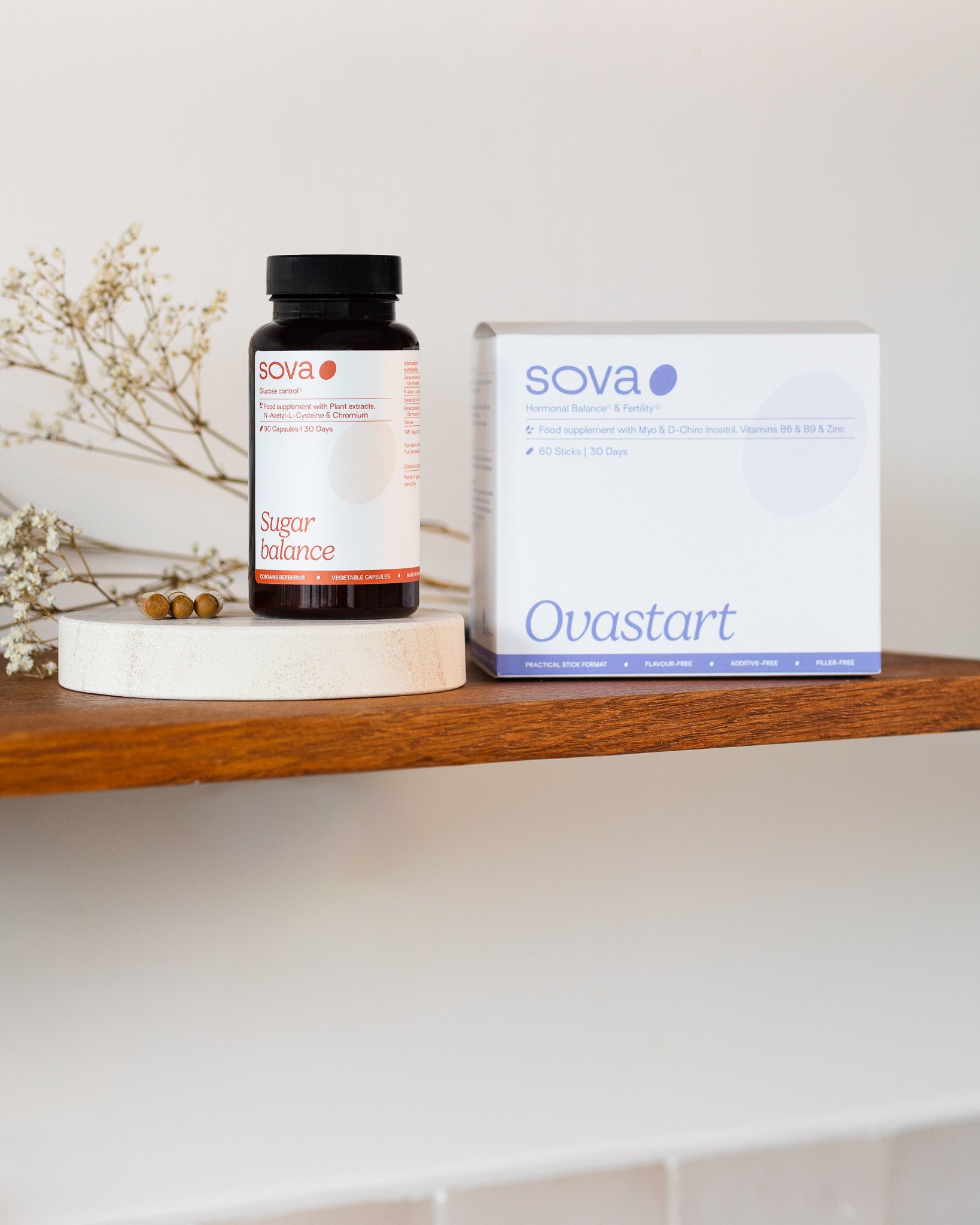
The Hormone Balance Supplements Built for PCOS - Two Products, One Complete System












